
Passwater:Dr. Traber, your discovery of the function of the tocopherol transfer protein (TTP) has enabled us to make some very important conclusions about the basic biochemistry of vitamin E. Based on what we have discussed in the previous two columns, are the following statements true? 1. The chemical form of vitamin E that is an essential nutrient for humans is alpha-tocopherol, and alpha-tocopherol only. The beta, delta and gamma forms are not essential for humans and are not retained in the body.2. No matter which form of the alpha-tocopherol is ingested orally—either the free form or esters like acetate or succinate—it will end up in the free form. This is because the free form doesn’t need conversion and digestive enzymes in the intestinal tract will convert the esters into the free form.3. There are no known clinical benefits of one vitamin E ester (such as alpha-tocopheryl acetate or alpha-tocopheryl succinate) over the other as they are both converted back to free vitamin E (alpha-tocopherol) in the digestive tract. 4. The “free” alpha-tocopherol is absorbed into the bloodstream and then transported to the liver.5. In the liver, the alpha-TTP selects the alpha-tocopherol for transfer to the plasma. Chemically, the form known as R,R,R-alpha-tocopherol (naturally found in plants), as well as the other three “2R” forms of alpha-tocopherol, which are known as R,R,S-alpha-tocopherol, R,S,R-alpha-tocopherol and R,S,S-alpha-tocopherol are the only four forms of alpha-tocopherol known to be transported and conserved by alpha-TTP. Alpha-TTP does not select the four “2S” forms of alpha-tocopherol present in synthetic alpha-tocopherol, or the beta-, gamma- and delta-tocopherol forms found in food.
Traber: Yes, that’s an accurate review.
Passwater: The discovery of vitamin E by Drs. Herbert McLean Evans and Katherine Scott Bishop did not seem to create much interest in doing more vitamin E research for a long time. Their discovery was related to vitamin E being required for fertility and gestation. Further studies with humans would seem to border on unethical, but farmers would benefit from such studies in farm animals. Even the horse racing industry would benefit. However, obtaining research funds would not be easy.
The major research on vitamin E seemed to be that of Dr. Max Horwitt in “The Elgin Project” in the late 1950s and early 1960s, which found that polyunsaturated fats increase the need for vitamin E in humans although vitamin E still was not recognized as being essential for humans (1–3). Dr. Horwitt discussed his early research in our November 1992 column on vitamin E and the RDA (4).
It wasn’t until the late 1960s that the research turned again to fertility studies and it was found that hemolytic anemia in premature infants given oxygen and/or polyunsaturated fats benefitted from vitamin E (5, 6).
Traber: Vitamin E is critical for the embryo. As I mentioned in Part 2, we use the zebrafish embryo because they are great models for studying embryogenesis. They don’t have the ethical and logistic issues that you have cited for human and rodent studies. As I mentioned in Part 2, zebrafish have many genes in common with human beings, so researchers often study them to gain insights into human disorders and conditions.
Our zebrafish embryo studies have shown that “knockdown” of alpha-TTP (preventing alpha-TTP production in the zebrafish) results in 100% death of the embryos within 24 hour. Thus, we now know that vitamin E is necessary for the development of the neural tube and the brain. Interestingly, this timing in zebrafish embryos takes place at the same times as “fetal resorption” in vitamin E deficient rats.
Passwater:So far, we have discussed only the nutritional requirement for vitamin E in fertility. Isn’t there more? Haven’t you also determined that alpha-tocopherol is nutritionally essential for normal brain development and function?The average intake of alpha-tocopherol from food for U.S. adults is 7.2 mg/day. This level is well below the RDA of 15 mg/day of alpha-tocopherol.
Regarding brain health beyond nutritional requirements, several researchers are looking into possible supranutritional levels of vitamin E and cognitive function, neurological deterioration and even Alzheimer’s disease. What is your research with zebrafish finding out about vitamin E and brain function?
Traber: It is complicated! It turns out that the brain accumulates long-chain omega-3 fatty acids, specifically docosahexaenoic acid (DHA). We found that adult fish fed a vitamin E-depleted diet for over a year had less DHA in their systems, which was not surprising since DHA is easily oxidized and vitamin E is known to protect DHA.
More importantly, we found that the adult zebrafish brain was depleted in a specific phospholipid-containing DHA, called DHA-PC, which is a critical part of the cellular membrane of every brain cell (7). This fat has been described as an important biomarker of Alzheimer’s in elderly humans. Wow! Who would have guessed that low blood DHA-PC is an indicator of Alzheimer’s disease in humans and low DHA-PC is found associated with low vitamin E levels in zebrafish brains?
Our studies have also shown that the vitamin E-deficient zebrafish are deficient in compounds called “lyso PLs,” which deliver DHA into the brain.
Passwater:Certainly an interesting connection. You have shown that vitamin E is essential to the developing brain and to protecting it throughout life. Other researchers are investigating vitamin E in Alzheimer’s patients to see if it can help. Protecting the brain is one thing, but undoing damage that has already occurred in the brain can be something else. Studies with 2,000 mg of vitamin E daily have been shown to slow the progression of the disease. Let’s take a closer look next month. But, for now, let’s stay with the essential nutritional role of vitamin E and the brain.
Doesn’t your latest research change the description of vitamin E’s role to specifically include fertility and brain development and function?
In Part 1, you said, “the major function of vitamin E appears to be that of a fat-soluble, chain-breaking antioxidant that protects polyunsaturated fatty acids within membranes and lipoproteins. This means that vitamin E protects cell membranes and lipoproteins from oxidative damage due to oxygen radical and other reactive oxygen species attack.”
This is a general activity. Shouldn’t we add the specific functions that you have established as being examples of specific functions of vitamin E to clarify its role?
Traber: Well, we are looking for specific examples in the body for how vitamin E functions as a fat-soluble, chain-breaking antioxidant. We know vitamin E acts as an antioxidant in the test tube. Now, we can point out specific examples of how fats are not protected when not enough vitamin E is present.
Passwater: Somewhere along the way, it seems that the public confused research with vitamin E and fertility with virility. All of a sudden, vitamin E became “sexy.”
Traber: Well, we hope it is sexy enough to get my grant proposal on vitamin E deficient zebrafish embryos funded!
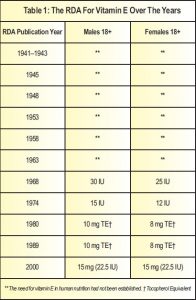
Passwater:We hope so, too. Vitamin E was not universally considered essential for humans until about 1966. The RDA was not established until 1968. The RDA has changed over the years, but not dramatically. Please see Table 1, which shows the vitamin E RDA over the years.
How does the vitamin E RDA compare to actual intakes?
Traber: In the United States, the average intake of alpha-tocopherol from food (including enriched and fortified sources) for adults is 7.2 mg/day (8). This level is well below the RDA of 15 mg/day of alpha-tocopherol. All of our work has consistently suggested that the recommendation is correct, despite the fact that dietary surveys suggest that more than 90% of Americans do not consume the recommended amount, or even 12 mg alpha-tocopherol (9).
Passwater: You have served on the scientific panel that sets the official RDA (DRI). It has been difficult to assess just how much vitamin E people should consume when we may not fully understand exactly all of the biochemical functions of vitamin E in the body.
For decades, we have relied on an assumption or the need for vitamin E to prevent undesirable oxidation and free radical formation from polyunsaturated fats. The assumption was that since we don’t recognize any overt vitamin E deficiency diseases, then the population must have been consuming adequate amounts of vitamin E. So, all that needs to be done is to calculate how much vitamin E is in the American diet and divide that by the population to get the number.
This is not very scientific, but a reasonable first estimate in the absence of scientific data. As mentioned earlier, the Elgin Project, headed by Dr. Horwitt, was the first study to approximate vitamin E needs indirectly by measuring the oxidation of polyunsaturated fats. Now you are working on the biomarker called alpha-CEHC as a better indicator. What is the basis of using alpha-CEHC (tetra-methyl carboxyethyl hydroxychroman) as a marker of vitamin E adequacy?
Traber: Alpha-CEHC is a metabolic product of the phytyl tail of alpha-tocopherol. When you have enough vitamin E, the body gets rid of the extra (10). This process is good because vitamin E doesn’t accumulate like some other vitamins, such as vitamin A.
Since alpha-CEHC is excreted in the urine, we can do a urine test to measure how much alpha-CEHC is present. We are now using deuterium-labeled vitamin E to demonstrate how much of a dose gets converted and excreted. We are hopeful that this information will be useful to the next committee to set vitamin E requirements.
Passwater:Before 2000, non-alpha-tocopherol isomers (beta-, gamma-, and delta-tocopherols) were thought to have some vitamin E activity. This is now considered incorrect. Due to the number of methyl groups on the head (ring structure) of the vitamin E molecule, they do not seem to fit into alpha-TTP as a perfect “hand and glove” match. After the 2000 DRI publication, these non-alpha-tocopherols were not assigned any vitamin E activity. Only alpha-tocopherol is designated as vitamin E. At one time, they were each assigned relative activity values. Is this still the situation?
Traber: I can only speculate because these studies are fairly old and I did not carry them out. What I think is that there were alpha-tocopherol contaminants in the various “pure” vitamins used for treatment. As recently as 10 years ago, I could not purchase “100% gamma-tocopherol.” It was only sold as 97% with 3% contamination of alpha-tocopherol. When we made diets with 500 mg of gamma-tocopherol/kg, then we ended up with sufficient alpha-tocopherol to ruin tests of gamma-tocopherol function.
The assignment of vitamin E activity for the non-alpha-tocopherols was based on very old and crude studies. In my opinion, the alleged activity was likely due to having to use impure preparations of the various non-alpha-tocopherol isomers. The bioassay is a crude assay and the preparations were impure.
Thus, the non-alpha-tocopherol samples tested probably contained enough alpha-tocopherol to account for much of the observed activity.
Note that the various forms of vitamin E are not interconverted. The non-alpha-tocopherol forms are rapidly metabolized to CEHCs and excreted. Some interesting studies claim activity of these metabolites, but these are not vitamin E activities. Rather, they are potential health benefits of non-alpha-tocopherol forms.
Passwater:At what ages and conditions is vitamin E intake the most important?
Traber: My guess, again based on our zebrafish work, is that women BEFORE they are pregnant need sufficient vitamin E. The vitamin E is necessary to protect DHA, a highly polyunsaturated fatty acid that is needed both for brains and eyes, really all of the nervous system in the developing fetus.
Passwater:The European Food Safety Authority issued a report last July stating that there was no apparent deficiency of vitamin E in the EU, and further stating that the DRV for Pregnant and Lactating Women should be eliminated, as there was no evidence of increased need for vitamin E in pregnant or lactating women (11). Any comment?
Traber: I think they only will be convinced by data, so I keep working on mechanistic data to show precisely why vitamin E is critical for embryonic development. And keep in mind that the breast-fed baby only gets alpha-tocopherol from mother’s milk, so the baby is depleting the mother’s vitamin E. I think it is clear that lactating mothers really need sufficient vitamin E!
Passwater:Has the misguided emphasis on low-fat diets been a contributing factor in Americans falling short of the vitamin E DRI?
Traber: Really, people need to eat nuts and seeds, whole grains and olive oil, which are not popular foods. The other solution is to do what the nutrition community did 100 years ago and recognize that fortifying food with B-vitamins was simpler than changing people’s eating habits. Since that hasn’t happened yet, the solution is to take a vitamin pill.
Passwater:Would vitamin E supplements be a logical and acceptable way to help Americans obtain the recommended amount of vitamin E?
Traber: I recommend multivitamins because I think most people’s diets are not nutritionally balanced. In addition, I think eating lots of vegetables and fruits is a good idea. I think we have overlooked the importance of an adequate intake of vitamin K. That comes from green leafy vegetables like kale, spinach, collard greens—you get the idea. Surprisingly, many multivitamins don’t contain vitamin K!
Passwater:We certainly want to discuss your research in balancing vitamin E and vitamin K in an upcoming column. Also, you have published that according to in vitro (cell culture) studies, vitamin E appears to have health benefits beyond the essential nutritional role(s).
Some suggest that what is essential in the overall scheme of nature is for our species to propagate more so than what amount of an essential nutrient also produces better health. It is argued that what is important in the long run is that we reproduce, but it is not so important that we live long lives. Vitamin E appears to be involved in immune function, cell signaling, regulation of gene expression and other metabolic processes (12). The DRI Committee, of which you were a member, has published that vitamin E has been shown to inhibit the activity of protein kinase C, an enzyme involved in cell proliferation and differentiation in smooth muscle cells, platelets and monocytes (13).
Let’s chat about cognitive function and Alzheimer’s disease and some of the “non-essential” roles for vitamin E in the next column. For now, thank you for once again informing us about the latest research in vitamin E nutrition.
In review, the major function of vitamin E appears to be that of a fat-soluble, chain-breaking antioxidant that protects polyunsaturated fatty acids within membranes and lipoproteins. This means that vitamin E protects cell membranes and lipoproteins from oxidative damage due to oxygen radical and other reactive oxygen species attack. Dr. Traber’s research has shown specific essential needs for vitamin E in embryo development and brain cell health. Only the alpha-tocopherol form of vitamin E is nutritionally essential for humans, but research is still examining possible clinical roles for vitamin E beyond its essential nutritional roles. The known essential nutritional requirement for alpha-tocopherol is 15 mg, yet more than 90% of the American population does not even reach 12 mg in their diet (9).WF
Dr. Richard Passwater is the author of more than 45 books and 500 articles on nutrition. Dr. Passwater has been WholeFoods Magazine’s science editor and author of this column since 1984. More information is available on his Web site, www.drpasswater.com.
References1. M.K. Horwitt et al., “Effects of Limited Tocopherol Intake In Man With Relationship To Erythrocyte Hemolysis And Lipid Oxidations,” Amer. J. Clin. Nutr. 4: 408 (1956). 2. M.K. Horwitt, “Vitamin E and Lipid Metabolism In Man,” Amer. J. Clin. Nutr. 8: 451 (1960). 3. M.K. Horwitt, “Interrelations Between Vitamin E And Polyunsaturated Fatty Acids In Adult Men,” Vitamins Hormones 20: 541 (1962). 4. R.A. Passwater, “Vitamin E and the RDA,” WholeFoods Magazine (November 1992). 5. H. Hassan et al., “Syndrome in Premature Infants Associated With Low Plasma Vitamin E Levels And High Polyunsaturated Fatty Acid Diet,” Amer. J. Clin. Nutr. 19: 147–57 (1966). 6. F.A. Oski and L.A. Barness, “Vitamin E Deficiency: A Previously Unrecognized Cause Of Hemolytic Anemia In The Premature Infant,” J. Pediatr. 70, 211–220 (1967). 7. J. Choi, et al., “Novel Function Of Vitamin E In Regulation Of Zebrafish (Danio Rerio) Brain Lysophospholipids Discovered Using Lipidomics,” J. Lipid Res. 56 (6), 1182–1190 (2015). 8. V.L. Fulgoni, et al., “Foods, Fortificants, And Supplements: Where Do Americans Get Their Nutrients?” J. Nutr. 141(10), 1847–1854 (2011). 9. M. Traber, “Vitamin E Inadequacy in Humans: Causes and Consequences,” Adv. Nutr. 5, 503–514 (2014). 10. M. Schultz et al., “Novel Urinary Metabolite Of Alpha-Tocopherol Alpha=CEHC As An Indicator Of An Adequate Vitamin E Supply?” Amer. J. Clin. Nutr. 62, 1527S-1534S (1995). 11. A-R Harrison-Dunn, “EFSA on Vitamin E:’Pregnant and Lactating Women Don’t Need More,” July 10, 2015, www.nutraingredients.com/Regulation-Policy/Pregnant-and-lactating-women-don-t-need-more-vitamin-E-EFSA, accessed May 24, 2016. 12. M.G. Traber, “Vitamin E,” in M.E. Shils, et al., eds. Modern Nutrition in Health and Disease. 10th ed. (Baltimore, MD: Lippincott Williams & Wilkins, 2006; 396-411). 13. Food and Nutrition Board, Institute of Medicine, Vitamin E. Dietary Reference Intakes For Vitamin C, Vitamin E, Selenium, And Carotenoids (Washington, D.C.: National Academy Press; 2000: 186–283).
Published in WholeFoods Magazine July 2016










