Passwater:Dr. Traber, last month we may have surprised some of our readers with the news that several popular supplements such as “400 IU vitamin E” capsules and “1,000 IU vitamin D” capsules will disappear by 2018 as the U.S. Food and Drug Administration (FDA) adopts the recommendations of the 2000 DRI Committee to label supplements by weight rather than by units of activity. The vitamins will still be available, but their labels will change in what could be a very confusing manner at first. The changes are good because they will put the FDA completely in line with all of the 2000 DRI recommendations for vitamin E.

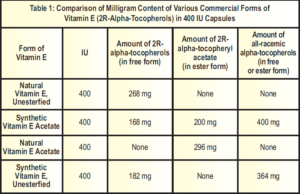
Traber: It will be interesting to see how the dietary supplement industry handles these changes. If we knew, we could start educating consumers now on what the differences mean. Presently, capsules labeled as containing 400 IU of natural unesterfied vitamin E include 268 mg of vitamin E (2R-alpha-tocopherols) as RRR-alpha-tocopherol.
However, a 400-IU capsule of synthetic vitamin E acetate offers only 180 mg of vitamin E as 2R-alpha-tocopherols, which is contained in the 400 mg of all-rac-alpha-tocopherol. These differences made it convenient for the consumer to purchase 400 IU of vitamin E, but also made it confusing since the activity contained in the 400 IU was estimated incorrectly. The new information on how the body recognizes vitamin E allows for scientists to confidently change the units.
What will manufacturers decide to offer as the new equivalent of the former 400-IU capsules? Will the quantities be adjusted slightly to yield round numbers so that the equivalent unesterfied natural vitamin E is labeled 300 mg and synthetic vitamin E acetate 200 mg?
Passwater:Please note that we chose the forms of vitamin E that we feel are the most popular forms of 400 IU of vitamin E—the unesterfied form for natural vitamin E and the acetate form for synthetic vitamin E—because this is what most consumers will be looking for. It’s not exactly the same as comparing apples to apples and oranges to oranges, but the differences are very minor. More exacting conversions are given in Table 1.
 The change from units of activity to a weight basis is desirable to clarify several issues about vitamin E as explained in the 2000 DRI report. It seems that many people and even government agencies have taken a while to adjust to the 2000 DRI report. You were a member of that committee. What is your reaction to everyone taking so long?
The change from units of activity to a weight basis is desirable to clarify several issues about vitamin E as explained in the 2000 DRI report. It seems that many people and even government agencies have taken a while to adjust to the 2000 DRI report. You were a member of that committee. What is your reaction to everyone taking so long?Traber: I think it is very important to go slowly when making changes from the status quo to what you think may be better. Keep in mind we are not just talking about label changes for vitamin E, but for all of the nutrients, both macro and micro. This process starts with adjusting the Dietary Reference Intakes, through multiple levels of scrutiny, and getting input from nutrition scientists, the public and industry and various government groups. The final decision of what goes on the label is intended, I think, to provide the public with information that will help them choose a better diet. It is also clear that what various people think is a better diet is not ever unanimous!
Passwater:The reasons for the change for vitamin E is reviewed in the following points that we have been emphasizing in our discussion:
• The chemical form of vitamin E that is an essential nutrient for humans is alpha-tocopherol and alpha-tocopherol only. The beta, delta and gamma forms are not essential for humans and are not stored in the body.
• No matter which form of alpha-tocopherol is ingested orally—unesterfied “free,” acetate or succinate—the intestinal tract will hydrolyze the esters and absorb the free form. Remarkably, all of the various vitamin Es (tocopherols and tocotrienols) are equally well absorbed.
•There are no known clinical benefits of one vitamin E ester (such as alpha-tocopheryl acetate or alpha-tocopheryl succinate) over the other as they are both converted back to free vitamin E (alpha-tocopherol) in the digestive tract.
• All of the vitamin E forms are transported to the liver, where the alpha-tocopherol transfer protein (alpha-TTP) selects only 2R-alpha-tocopherol for re-secretion back into the blood stream. The alpha-TTP works in the liver only and is not in the blood.
Alpha-TTP will transfer the natural form of alpha-tocopherol (found in nature and made by plants), which is chemically known as the R,R,R-alpha-tocopherol. Alpha-TTP will also transfer some of the synthetic forms of alpha-tocopherol, which are chemically known as 2R-alpha-tocopherols. 2R-alpha-tocopherols are present in all rac alpha-tocopherol and include R,R,R-; R,R,S- R,S,R- and R,S,S- alpha-tocopherol. (Please see Figure 1.)
Dr. Traber, have the food values also been recalculated based on the 2000 DRI recommendations or should they be recalculated if they haven’t been? The non-alpha isomers of tocopherol—especially gamma tocopherol, the most prominent form in American diets—are not vitamin E as pointed out above and accepted by the National Academy of Sciences and the FDA. Yet, most food values have considered all tocopherols as vitamin E in the past.
Traber: The U.S. Department of Agriculture food tables, called nutrient composition tables, have the correct concentration of vitamin E in foods. Of course, these are always being updated because our food supply is constantly changing. The version I am checking as we chat was updated in May 2016. Readers might enjoy seeing their tax dollars at work by going to https://ndb.nal.usda.gov and looking up a few of their favorite foods.
Passwater:We have already discussed that most people fail to get the recommended amount of vitamin E. The nutritional requirement for vitamin E is 15 mg (22.5 IU), yet about 90% of the American population does not even reach 12 mg in their diet. In addition, a recent publication in the International Journal for Vitamin and Nutritional Research indicates that only one-fifth of the global population does not get the recommended amount (1). Your research suggests that obese people—especially those with metabolic syndrome—need more vitamin E. It’s estimated that about one-third of U.S. adults have this syndrome. Since the definition of metabolic syndrome is having at least three of five issues of health concern—excess abdominal fat, high blood pressure, low HDL cholesterol and/or high levels of blood sugar and triglycerides—individuals especially need vitamin E because they are at increased risk for heart disease, diabetes, Alzheimer’s disease and cancer.
Traber: Obese persons with metabolic syndrome face a quandary concerning vitamin E. Their weight and other problems associated with obesity increase oxidative stress, which increases the need for vitamin E. Even if their dietary vitamin E were adequate, adequate amounts of the vitamin may not find its way into the tissues where it is needed.
Last year, we reported in the American Journal of Clinical Nutrition that metabolic syndrome patients had lower levels of two lipoproteins (lipoproteins consist of both proteins and fats which allow fats to move through watery fluids outside cells); one in the liver and the other in the small intestine (2). Intestinal lipoprotein aids vitamin E absorption and liver lipoprotein aids fat and vitamin E secretion into the blood.
Passwater:Nutritionists often lose sight of the fact that it is neither how much of a nutrient that goes into the mouth that counts, nor is it what gets absorbed and transported in the blood. What counts is how much gets into the cells of the tissues that need the nutrients.
Why are the obese—especially those with metabolic syndrome—inefficient at getting vitamin E from the blood into the cells?
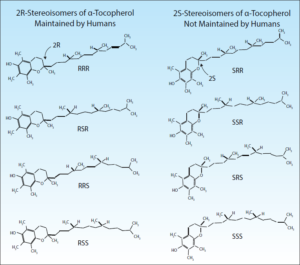
vitamin E is 50% “2R” and 50% “2S,” however, the “2R” is not all RRR-alpha-
tocopherol. Synthetic vitamin E also contains three additional “2R” structures: the “RSR,” “RRS” and “RSS” structures.
Traber: Remember, we were talking about the important role the liver plays in selecting alpha-tocopherol and no other forms of vitamin E for secretion into circulation. A complication of metabolic syndrome is non-alcoholic fatty liver disease and you can tell by the name of this disease that the liver accumulates excess fat. The extra fat may prevent the vitamin E from being resecreted into the bloodstream. Instead of being available to the tissues, it is stuck in the liver. We are currently investigating this process, so stay tuned for the latest updates!
Passwater:You have noted that the structural similarities between vitamins E and K may present a problem if one is out of balance with the other. What are your concerns?
Traber: Vitamin K is an interesting nutrient because the body actually converts it to a form with an unsaturated tail, menaquinone-4. This latter form is present in the brain in high concentrations. Vitamin K is hard to study in humans because the tissues that are important, the liver and the brain, are not easy to investigate. Since the body is smarter than the scientists in this case, I encourage everyone to eat lots of green leafy vegetables so you make sure you get your vitamin K!
Passwater: Amen! Your point that the body is smarter than the scientists studying it is well taken! In my case, I am reminded of this nearly every day as I continue to learn. I’ll bet you that this will be true for many more than 100 years from now.
Is there any other research that you can share with us that is in press and may be published soon?
Traber: We are actively looking at biomarkers of vitamin E status. Can we evaluate an individual’s vitamin E status just by measuring a simple biomarker? We are working on individualized vitamin E nutrition. Also, we are working on exactly why does an embryo die if it has inadequate vitamin E. In this case, we are using zebrafish embryos, which are routinely used in vertebrate development research.
Passwater:Dr. Traber, we thank you for your patience and time to improve our understanding of vitamin E. We will eagerly await your future research findings.WF
References1. P. Szabolcs, “A Systematic Review of Global Alpha-Tocopherol Status as Assessed by Nutritional Intake Levels and Blood Serum Concentrations,” Int. J. Vitam. Nutr. Res. 14, 1–21. (2016). 2. E. Mah et al., “a-Tocopherol Bioavailability Is Lower In Adults With Metabolic Syndrome Regardless Of Dairy Fat Co-Ingestion: A Randomized, Double-Blind, Crossover Trial,” A
 m. J. Clin. Nutr. 102 (5), 1070–1080 (2015).
m. J. Clin. Nutr. 102 (5), 1070–1080 (2015).Dr. Richard Passwater is the author of more than 45 books and 500 articles on nutrition. Dr. Passwater has been WholeFoods Magazine’s science editor and author of this column since 1984. More information is available on his Web site, www.drpasswater.com.
Published in WholeFoods Magazine September 2016









