In the 1970s, whenever I gave a lecture about my research, someone would inevitably ask me about vitamin E as a treatment for heart disease. The same was true when writers wrote about my research. In the early 1960s my research consisted essentially of laboratory animal studies of synergistic antioxidant nutrients in regards to increasing longevity, decreasing cancer incidence and protection from air pollution. I was researching vitamin E in some aspects of health, but I was almost constantly asked about vitamin E and heart disease, which was not part of my research. It became somewhat frustrating for two reasons; one, it had nothing to do with my research, and two, I didn’t know the answer. I finally realized that I had to look into the heart disease research so that I could give an informed answer.
I contacted a friend, Jud Ryon in Wilmington, Delaware. Jud was the 1944 president of the National Products Association (NPA). Jud was the first health food retailer to sell vitamin E supplements and he knew the Drs. Shute. Before Jud introduced pure vitamin E capsules, the best source of vitamin E available was wheat germ oil. Jud had read the 1948 Coronet magazine article about the research of the Drs. Shute and went to visit them to see for himself. In 1945, prior to the Coronet article, the Drs. Shute published the first scientific article claiming that supranutritional doses of vitamin E slowed down and even reversed heart disease (8). This publication was followed by peer-reviewed publications (9,10). The Drs. Shute had also reported in 1946, that vitamin E (alpha-tocopherol) improved impaired capillary permeability and low platelet counts in experimental and clinical thrombocytopenic purpura (11).
Dr. Wilfrid Shute wrote “Alpha tocopherol [vitamin E] in cardiovascular disease” in 1954 (Ryerson Press, Toronto, Canada) primarily for physicians. Dr. Evan Shute wrote “Your Heart and Vitamin E” in 1956 (Cardiac Society) primarily for the general population. Singularly and jointly, they wrote several books on vitamin E and heart health through the years. These books were responsible for the public’s association of vitamin E with heart health. My favorite was Dr. Wilfrid’s book written with my first editor, Harald Taub, “Vitamin E for Ailing and Healthy Hearts” (Pyramid House, 1970).
The Drs. Shute were clinical physicians and were trained to think primarily in terms of cure, rather than prevention or research. They recognized coronary thrombosis for what it is —blood clots forming in the coronary arteries that prevent blood from nourishing and oxygenating the heart. The blockage by the clots leads to death of tissue (infarct) in the heart (myocardium), hence the term myocardial infarction. The Drs. Shute knew that vitamin E helped keep the blood free-flowing and their observations convinced them that vitamin E would also help dissolve clots.
My October 1992 Vitamin Connection column with Jud Ryon details how Jud had vitamin E capsules made and introduced in the USA (12).
After his visit with the Drs. Shute, Jud stopped on his way home at the Vitamin Corporation of America in Newark, NJ, and ordered 100,000 tablets. All that was available at that time to the health food market was wheat germ oil.
The first vitamin E that was available in sufficient strength to be effective for most people with heart disease was Ephanol, a synthetic vitamin E made by a “tiny” apparatus at Hoffman-La Roche. However, this material was very expensive at the time. Soon thereafter, a natural vitamin E derived from vegetable oil became available from Distillation Products in Rochester, NY. This was stabilized as tocopheryl phosphate and was significantly less expensive. The Drs. Shute first used the synthetic vitamin E and then switched to the less expensive natural vitamin E when it became available.
As described in reference 12, within three weeks of advertising and selling vitamin E, the FDA raided Jud’s store and confiscated his stock and copies of the Coronet article. Their complaint was that vitamin E was not accepted as necessary in human nutrition.
I asked Jud to introduce me to the Drs. Shute. Later, Dr. Evan Shute was kind enough to write a review of my book, “Supernutrition For Healthy Hearts” (13) and we lectured together many times over the years in several countries. In 1978, Dr. Evan Shute’s son, Vere, wrote to me saying that not only did both Drs. Shute highly recommend my book, but that the Shute Institute provided patients with copies of both “Supernutrition: Megavitamin Revolution” and “Supernutrition For Healthy Hearts.”
The research of the Drs. Shute and their writings have been very important historically in creating an interest in vitamin E supplements in the general public. When I started writing and lecturing about my research that included vitamin E as an antioxidant, it was only natural for people to ask me about vitamin E and heart disease. So, I had to investigate further. First, I wanted to see if vitamin E actually helped the many people taking it based on the Drs. Shute advice.
As I am not a physician, but a research biochemist, the best way that I could investigate the relationship was to conduct an epidemiological or “population-based” study of any possible correlation. What I found and published in 1976 was that the longer people took sufficient quantities of vitamin E, the less heart disease they had as a group (14).
Epidemiological studies can establish association (correlation), but do not prove cause and effect. For example, when you see a crowd of people holding open umbrellas over their heads, it’s not the umbrellas that caused the rain.
Association studies are properly used to see if there is a possibility of a relationship and if there is, then a study can be designed to test causation or not. Merely conducting additional correlation studies is a waste of time and money because no matter how many there are, they can’t prove a thing. What is often overlooked, however, is that a lack of association does prove that it is not a cause. Epidemiological studies can indirectly support the premise because if correlation is not found, then the premise is not true. A lack of association disproves the theory.
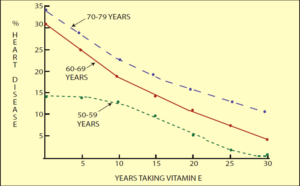
With that said, my 1976 epidemiological study among 17,894 adults aged 50–90 found that the length of time taking vitamin E was more important than the dose, but both time and dose were critical (please see Figure 1) (14). It wasn’t surprising that both were important because vitamin E as a nutrient needs time to help repair the body at the cellular level. Drugs may act to change symptoms quickly, but nutrients act at the cellular level. In my study, the reduction in heart disease incidence was not seen until two years after starting vitamin E supplements. held a news conference at the National Press Club in Washington to give the data and results of my study to science reporters (15). In spite of the conference being held on Christmas Eve, it was well attended and well-reported. On Christmas, Lasker Award winner and national syndicated science writer Judith Randall’s (New York Daily News) article was carried in hundreds of newspapers. Also, nationally syndicated writer Susan Fogg’s (Globe-Democrat National Service) article “Expert links low heart disease rate, vitamin E” was published in many more papers. I thought that this made a nice Christmas present for everyone.
My study was the first to suggest that vitamin E could help prevent heart disease. This is different than the Drs. Shute studies using vitamin E to help treat existing heart disease, and also different than studying the essential nutrient role of vitamin E. Fortunately, many people have taken advantage of this information to reduce their risk of early heart disease while the scientific community continues to debate and deny.
As I published in “Supernutrition For Healthy Hearts,” two groups in the study illustrate the importance of time as well as dosage (14). The study found that the Spearman-Rho association between length of time taking vitamin E and freedom from heart disease was 0.96 where 1.00 would be perfect association. This correlation is significantly different from chance at the 0.01 level p=0.01.
One group in the study consisted of those who had taken 400 IU or more of vitamin E daily for ten years or more. The study included 2,508 such persons between the ages of 50 and 98 years. Normally, based on U.S. Department of Health, Education and Welfare (now HHS) figures (HRS 74-1222), it would be expected that 836 of the 2,508 would have heart disease. Instead there were fewer than 10% of the expected number. For this group, it was concluded that taking vitamin E supplements of 400 IU or more for ten years or more was strongly associated with the reduction of the incidence of heart disease prior to 80 years of age to less than 10% of the present rate (32 per 100 people) to three per 100 people.
A second group of 1,038 people had taken 1,200 IU or more of vitamin E for four years or more. Among this group, it would be expected to have 323 persons suffering from heart disease. But the actual number in the study was seven.
Getting back to the Drs. Shute, among those in the survey who already had heart disease at the time of the survey, 80% reported that vitamin E helped their condition measurably. Some people reported that before they started taking vitamin E, they were taking as many as 18 or more nitroglycerine pills daily for their angina pectoris. Angina pectoris is the pain or pressure felt in the chest due to insufficient blood and oxygen reaching the heart. Soon after they began to take vitamin E supplements, they were able to discontinue taking nitroglycerine pills. Some felt so good they also gave up taking their vitamin E supplements, but their angina pains would return within a few weeks or months. These are anecdotal reports and they may be influenced by placebo effect. However, the main focus of the study was heart attack incidence which is not influenced by placebo effect.
An interesting sidelight is that in 1982, Dr. Linus Pauling and Dr. James Enstrom used my database to study mortality in a select group of elderly Californians (16).
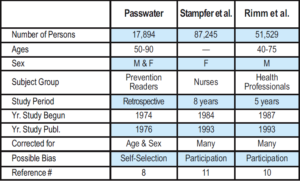
Nearly two decades later, two groups at Harvard published epidemiological studies in the New England Journal of Medicine, also suggesting that vitamin E was associated with the prevention of heart disease. An intake in adequate amounts over an adequate period of time reduced the risk of heart disease. In a prospective study of 51,529 male health professionals who were 40 to 75 years of age called “The Health Professionals Follow-up Study,” Eric Rimm, Sc.D.’s group at Harvard found that those who consumed 100 IU or more of vitamin E daily for two years or more had a 37% reduction in heart disease (17).
The study also found that men who took vitamin E supplements for 10 or more years had a relative risk of 0.65 compared with nonusers. That’s a 35% reduction in incidence. This confirms my study that showed length of time taking vitamin E supplements is more important than the dosage, although both are important. When the length of time is greater, it is probable that the supplementation started at a younger age and thus, started protection earlier before irreversible damage occurred.
In the Health Professionals Follow-up Study, compared to men in the lowest quintile group for vitamin E intake, the men in the highest quintile group had a 41% reduction in coronary disease (relative risk of 0.59; P for trend = 0.001). For fatal coronary disease or nonfatal myocardial infarction, the relative risk between the highest and lowest quintile groups for vitamin E intake was 0.63, and for bypass grafting or angioplasty the relative risk was 0.68.
Regarding overall mortality, the relative risk was 0.78 (22% reduced mortality rate) when highest and lowest quintile groups for vitamin E intake were compared.
The researchers remarked, “These data are compatible with the hypothesis that an increased intake of antioxidants, primarily as vitamin E, is associated with a reduced risk of coronary disease…Our findings for vitamin E are consistent with correlations between serum vitamin E levels and coronary mortality rates and reduced serum levels of vitamin E in patients with angina. Most notably, the associations we found for vitamin E supplements were remarkably similar to those found among women in the Nurses' Health Study. Vitamin E appeared to reduce atherosclerosis in a small experiment in monkeys and to decrease the rate of restenosis among patients after angioplasty.”
In the same issue of the 1993 New England Journal of Medicine, a study of 87,245 women, by Meir Stampfer, M.D., Ph.D.’s group at Harvard found that women who took 100 IU or more of vitamin E daily for two years or more had a 46% reduced risk of heart disease (18). The study, a part of the Nurses’ Health Study, also reported that after adjustment for age and smoking status, both vitamin E supplements and multivitamins were associated with a lower risk of major coronary disease. The relative risk for women who took multivitamins was 0.78 (22% reduced risk) and for those who took vitamin E supplements it was 0.57 (43% reduced risk), as compared with the risk in those who took neither.
It is important to note that the researchers reported, “Users of vitamin E for less than two years had no significant reductions in risk.” This is in full agreement with my earlier study and the Health Professionals study. Because of this important time factor, it is apparent that any study of vitamin E and heart disease of less than two years’ duration is meaningless. The researchers also reported, “Use of vitamin E for two or more years, however, was associated with a decrease in risk of 41%”
The researchers concluded, “In this large prospective study, we observed a risk of major coronary disease among women who took vitamin E supplements that was about 40% lower than the risk in women who did not take these supplements; this association changed little after adjustment for coronary risk factors and the intake of other dietary antioxidants.” The operative words in these studies are adequate dosage and time. Less of either was not found to be effective.
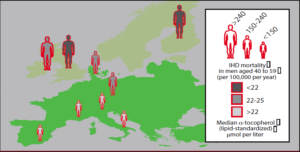
Prior to the 1993 Harvard studies, a European epidemiological study added support to the premise that vitamin E was protective against heart disease. In 1991, Dr. Fred Gey of the University of Berne, Switzerland, and colleagues published the study of persons in 18 different populations in Europe who participated in the World Health Organization’s Monitoring Trends in Cardiovascular Disease (WHO/MONICA) study. There was a seven-fold difference in heart disease mortality between populations. The study showed that a deficiency of vitamin E was the major and most reliable indicator of heart disease risk (Please see Figure 2) (19). Not dietary cholesterol, not dietary fat — but low levels of vitamin E in the blood.
This study found that low levels of vitamin E predicted a heart attack 62% of the time, while high blood cholesterol was predictive only 29% of the time and high blood pressure was predictive only 25% of the time.
Also in 1991, Dr. Gey and his colleagues published a case-controlled study of angina pectoris patients and vitamin E plasma levels (20). The case-controlled study examined the relation between risk of angina pectoris and plasma concentrations of vitamin E. Angina pectoris pain is the most common complaint of heart disease patients and has been the focus of most cardiologists including the Drs. Shute. The study compared 110 cases of angina and 394 controls. Plasma concentrations of vitamin E were found to be significantly inversely related to the risk of angina. Vitamin E remained independently and inversely related to the risk of angina after adjustment for age, smoking habit, blood pressure, lipids, and relative weight. The adjusted odds ratio for angina between the lowest and highest quintiles of vitamin E concentrations was 2.68 (p=0·02). This means that those with the lowest dietary levels of vitamin E had nearly three times the risk of angina. The researchers concluded, “These findings suggest that some populations with a high incidence of coronary heart disease may benefit from eating diets rich in natural antioxidants, particularly vitamin E.”
A 1991 study in Poland found that vitamin E blood levels were lower in angina patients than in healthy controls (21).
In 1992, The Scottish Heart Study found that the risk of coronary heart disease was significantly lower in the highest quintile of dietary vitamin E intake in 10,359 persons aged 40–59 years (22). The researchers concluded, “The results suggest that high dietary intake of the antioxidant vitamins may reduce risk of CHD, particularly in men.”
A study of nineteen Western European and five non-European countries in 1994 called “The European Paradox,” found that vitamin E was strongly related to rates of coronary heart disease (CHD) across Europe. Longitudinal analyses of nutrient supplies and death rates within each country from 1970 to 1987 showed that for the majority of countries there was an inverse association between intake of vitamin E and CHD. The researchers concluded, “Dietary alpha-tocopherol may provide at least as good an explanation as does wine for the paradoxically low rates of CHD in several European countries which have a relatively high saturated fatty acid intake” (23).
In 1994, a Finnish study found that the risk of fatal heart disease was lower in persons consuming more vitamin E. In this study, the relation between the intakes of dietary vitamin E and the subsequent coronary mortality was studied in a cohort of 5,133 Finnish men and women aged 30–69 years and initially free from heart disease. Altogether, 244 new fatal coronary heart disease cases occurred during a mean follow-up of 14 years beginning in 1966–1972. An inverse association was observed between dietary vitamin E intake and coronary mortality in both men and women with relative risks of 0.68 (p for trend = 0.01) and 0.35 (p for trend < 0.01), respectively, between the highest and lowest tertiles of the intake. (24)
Another Finnish study was published the following year in 1995 showing an inverse association of blood vitamin E levels with cardiovascular heart disease (25).
Also in 1995, the relationship between vitamin E intake and the progression of coronary artery disease (CAD) was evaluated in 156 middle-aged men (40 -59 years of age) in the U.S. having previous coronary bypass surgery (26). This study was part of the Cholesterol Lowering Atherosclerosis Study (CLAS) and was reported in the Journal of the American Medical Association. It found that men who took at least 100 IU per day from supplements showed significantly less CAD progression than men who took less vitamin E. The researchers concluded, “These results indicate an association between supplementary vitamin E intake and angiographically demonstrated reduction in coronary artery lesion progression.”
Additionally, in 1995, a study in India examined blood levels of vitamin E, along with vitamins A and C found an inverse relationship between them and coronary artery disease (CAD) (27). The urban population studied is similar to that in developed countries. Vitamin E levels remained independently and inversely related to the risk of CAD after adjustment for age, smoking, diabetes, blood pressure, blood lipoproteins, and relative weight and body mass index. The adjusted odds ratios for CAD between the lowest and highest quintiles of vitamin E levels was 2.53.
In the same year, a study in Turkey found blood levels of vitamin E were lower in those with cardiovascular disease (28). The case-controlled study was controlled for potentially confounding parameters such as age, sex, smoking status, quetelet index (kg/m2), alcohol consumption, dietary intake and serum lipids.
In the following year (1996), a study of postmenopausal women found that the intake of vitamin E from food is inversely associated with the risk of death from coronary heart disease (CHD) (29). In the study, 34,486 postmenopausal women with no cardiovascular disease completed a questionnaire in early 1986 that assessed, among other factors, their intake of vitamin E from food sources and supplements. During approximately seven years of follow-up (ending December 31, 1992), 242 of the women died of coronary heart disease. Relative risk of death from CHD was 58% lower in the two highest quintiles of dietary vitamin E intake than in the lowest quintile. The researchers noted, “the effects of high-dose supplementation and the duration of supplement use could not be definitely addressed.”
Also in 1996, a study of 11,178 people aged 67 to 105 years by the U.S. National Institute of Aging found that vitamin E reduced the risk of coronary disease mortality by 47% (RR = 0.53; 95% CI: 0.34, 0.84) and risk of all-cause mortality by 34% (relative risk (RR) = 0.66; 95% CI: 0.53, 0.83) (30). Use of vitamin E at two points in time was also associated with reduced risk of total mortality compared with that in persons who did not use any vitamin supplements. Effects were strongest for coronary heart disease mortality which saw a 63% reduced risk (RR = 0.37; 95% CI: 0.15, 0.90). Cancer risk was reduced by 59% (RR for cancer mortality was 0.41 (95% CI: 0.15, 1.08). The researchers concluded, “These findings are consistent with those for younger persons and suggest protective effects of vitamin E supplements in the elderly.”
A 1996 Canadian study also found that vitamin E supplement users had a significantly lower risk of heart attacks (myocardial infarctions) and death due to heart disease (31). Also, persons who took vitamin E supplements had a significantly decreased risk of new heart disease events. This cohort study was conducted between 1985 and 1991 in Quebec City. In 1985, 2,313 men provided baseline information on vitamin supplement use and heart disease risk factors. Incidence of heart disease events were ascertained over the first five years of follow-up. The associations were stronger for heart disease death and myocardial infarction, two events assessed with high validity. The inverse association with heart disease was more consistent for vitamin E than for any other vitamin. The researchers concluded, “This study suggests that the inverse association between vitamin supplement use and IHD is real.”
The same year, a Swedish study added to the evidence that was so apparent to the Drs. Shute. The study examined the blood levels of vitamin E in young male survivors of heart attacks in relationship to the severity of their coronary artery disease (CAD) (32). The study found that lipid-adjusted blood and Low-Density Lipoprotein (LDL) vitamin E levels were significantly lower in patients with heart disease than in healthy controls. There was a significant inverse correlation between LDL vitamin E levels and the number and size of coronary lesions (plaque in the coronary arteries). The researchers concluded, “a low LDL vitamin E concentration might play a role in the development of stenoses in coronary arteries and may contribute to clinically manifest CAD.”
In 1997, an Austrian study found that vitamin E levels in the LDL of angina pectoris patients was also lower than those in healthy subjects (33).
In the following year (1998), a South African study compared plasma levels of vitamin E with coronary artery disease in men with those in healthy men. After adjusting for major risk factors, per-quartile decreases in blood vitamin E levels were associated with increased coronary artery disease risk. Decreased vitamin E concentrations are independently associated with increased risk of CAD independent from other CAD risk factors (34).
A 1999 review of the evidence in American Family Physician advised, “Recent studies show that supplementation with antioxidant vitamins E and C have benefits in CHD prevention. Current evidence suggests that patients with CHD would probably benefit from taking vitamin E in a dosage of 400 IU per day and vitamin C in a dosage of 500 to 1,000 mg per day. Clinicians may also want to consider vitamin supplementation for CHD prevention in high-risk patients.” (35)
A 2001 review published in the journal Atherosclerosis correctly pointed out that heart disease is an inflammatory disease involving a misbalance of the immune and redox homeostasis (36). The review examined the role of biology of atherosclerosis, and concluded that vitamin E has been shown to play a role in the initiation and progression of the disease. The researchers also pointed out that recent data reveals that the activities of vitamin E go beyond its redox function. They noted vitamin E can exacerbate certain processes associated with atherogenesis, and suggest that these two facets decide the clinical manifestation and outcome of the disease.
The case-controlled angina pectoris studies are very supportive of the teachings of the Drs. Shute and the reports from the existing patients in my 1976 study. As mentioned earlier, such epidemiological studies establish association (correlation), but do not prove cause and effect. However, they do support the premise because if correlation is not found, then the premise is not true. A lack of association disproves the theory.
Scientists look at large, randomized, placebo-controlled clinical trials (RCT) as their “Gold Standard” of evidence for cause and effect. RCT are usually very meaningful, but do they apply to nutritional studies in which the interaction of various nutrients cannot be examined? Some are quick to point out that RCTs of pharmaceutical treatment often do not lend support to these epidemiological dietary studies. I will be quick to point out that no RCT has proved that vitamin E does not reduce the incidence of heart disease when taken at sufficient dosage of 100 IU or more for a sufficient time of two years or more. It is easy for critics to wrongly dismiss all of the supportive evidence by quoting a couple of improperly-designed, non-supportive RCTs, but this is nonscientific.
RCTs are usually, but not always, relatively short-term studies due to expense and experiences with quick-acting pharmaceuticals. Often, the studies also give subjects powerful pharmaceuticals along with the nutrients thus masking and overwhelming any effect due to the nutrients alone. Please remember my earlier caution that since vitamin E doesn’t show benefit against heart disease until two years of usage, studies of vitamin E and heart disease of less than two years are meaningless.
Also, RCTs have the potential for masking beneficial effects in particular subgroups of the population (37).
The 2000 DRI states that “The hypothesis that reactive oxygen species and reactive species play a role in atherosclerosis rests on a solid basic science foundation and is strongly supported by studies in animal models. At the clinical level, a variety of correlational studies and studies of biochemical markers are consistent with the hypothesis. However, only four published large-scale, randomized, double-blind clinical intervention studies have tested the ability of vitamin E to prevent myocardial infarction. One of these, a secondary prevention trial supplementing with 400 or 800 IU of RRR-alpha-tocopherol was strongly positive” (38).
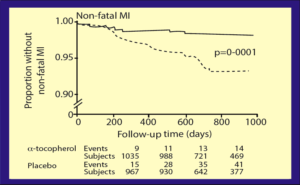
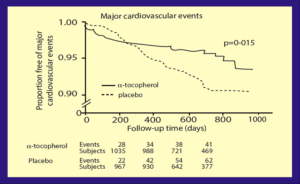
This clinical study referenced in the 2000 DRI was the 1996 double-blind, placebo-controlled, randomized, intervention clinical trial in England called the Cambridge Heart Antioxidant Study (CHAOS). Cardiac patients with angina pectoris (chest pains due to coronary artery disease) were treated with either a placebo or 400 IU or 800 IU of vitamin E, and the occurrence of heart attacks was monitored (39). The CHAOS study concluded that in patients with angiographically proven symptomatic coronary atherosclerosis, vitamin E treatment substantially reduces the rate of non-fatal heart attacks, with beneficial effects apparent after one year of treatment. (39)

In the CHAOS study, vitamin E treatment significantly reduced the risk of cardiovascular death and non-fatal heart attacks by 47% (relative risk 0.53, p=0·005). The beneficial effects on this composite endpoint were due to a significant reduction in the risk of non-fatal heart attacks by 77% (RR= 0.23 ; p=0·005.)
With this historical review, I do not imply that heart disease is caused solely by a vitamin E deficiency. There are important differences between the essential roles of a vitamin and ancillary adjunct roles. The same molecule can have several health functions, some of which are essential and some which are non-essential, but important to overall health. When considering a nutrient, one must be careful not to have the functional fixedness of Gestalt Psychology. Functional fixedness is a cognitive bias that limits a person to using an object only in the way it is traditionally used. A screwdriver is designed to drive screws, but it can also open jar lids and punch holes. Relatedly, in the absence of a screwdriver, a coin can be used.
Vitamin E, which has the specific antioxidant function of protecting cell membranes, can also function as a general antioxidant and have additional NON-SPECIFIC functions that can be shared with or replaced by other general antioxidants. Vitamin E is incorporated into lipoproteins and cell membranes, limiting LDL oxidation. In fact, vitamin E is the predominant antioxidant in LDL. Vitamin E also inhibits platelet activation and monocyte adhesion, but is this an “essential” role or just a beneficial role?
Alpha-tocopherol is essential to protect cell membranes, but according to the 2000 DRI, can also affect other mechanisms. The 2000 DRI states that vitamin E has been shown to inhibit the activity of protein kinase C, an enzyme involved in cell proliferation and differentiation in smooth muscle cells, platelets and monocytes (38).
Non-essential, but important, functions of vitamin E include better protection of the endothelial cells lining the interior surface of blood vessels against blood-cell components adhering to this surface. Vitamin E can reduce LDL oxidation and improve membrane stability. In the Nurses’ Health Study by Stampfer and colleagues, it was pointed out that “Rapidly growing evidence suggests that oxidation of LDL plays an important part in atherosclerosis.
As Steinberg et al. have found, oxidized LDL is taken up more readily than native LDL by macrophages to create foam cells. Also, oxidized LDL is chemotactic for circulating monocytes, and it inhibits the motility of tissue macrophages. It may also be cytotoxic to endothelial cells and may increase vasoconstriction in arteries. Oxidized LDL has been identified in atherosclerotic lesions, and elevated titers of circulating autoantibodies to epitopes of oxidized LDL are found in patients with atherosclerosis. Lipid peroxide concentrations have been found to be higher in patients with atherosclerosis. In addition, the susceptibility of LDL to oxidation was correlated with the severity of atherosclerosis.”
Vitamin E also increases the expression of two enzymes that suppress arachidonic acid metabolism, thereby increasing the release of prostacyclin from the endothelium, which, in turn, dilates blood vessels and inhibits platelet aggregation (38). Arterial stiffness is a precursor of heart disease (please see Figure 5) (40). Vitamin E has been shown to preserve arterial function and reduce arterial stiffness (41). There is indeed a solid biochemical basis as to how alpha-tocopherol (vitamin E) can help protect against heart disease. Overall, the subject remains controversial at best, but if examined in terms of differentiating long-term prevention from short-term treatment, th
 e picture may be clearer. WF
e picture may be clearer. WFDr. Richard Passwater is the author of more than 45 books and 500 articles on nutrition. Dr. Passwater has been WholeFoods Magazine’s science editor and author of this column since 1984. More information is available on his website, www.drpasswater.com.
References
- Passwater, R.A. New Evidence About the Safety of Vitamin E Supplements: An Interview With Manfred Eggersdorfer, Ph.D.Whole Foods (November 2015). https://wholefoodsmagazine.com/columns/vitamin-connection/new-evidence-about-safety-vitamin-e-supplements/
- Passwater, R.A. Toward A Better Understanding of Vitamin E Part 1: Clarifying Its Essential Vitamin Role. An Interview With Maret G. Traber, Ph.D. Whole Foods (May 2016) https://wholefoodsmagazine.com/columns/vitamin-connection/toward-better-understanding-vitamin-e-part-1-clarifying-its-essential-vit/
- Passwater, R.A. A Better Understanding of Vitamin E Part 2: “Natural-Source” and Synthetic Vitamin E. An Interview With Maret G. Traber, Ph.D. Whole foods (June 2016) https://wholefoodsmagazine.com/columns/vitamin-connection/better-understanding-vitamin-e-part-2-natural-source-and-synthetic-vita/
- Passwater, R.A. A Better Understanding of Vitamin E. Part 3: Recommended Nutritional Intakes and the Role of Vitamin E in Brain Health. Whole Foods (July 2016) https://wholefoodsmagazine.com/columns/vitamin-connection/a-better-understanding-of-vitamin-e/
- Passwater, R.A. A Better Understanding of Vitamin E. Part 4: FDA Changes the Traditional 400 IU Vitamin E Supplement; Brain Health and Alzheimer’s Disease Research, An Interview with Maret G. Traber, Ph.D. Whole Foods (August 2016) https://wholefoodsmagazine.com/columns/vitamin-connection/better-understanding-vitamin-e-2/
- Passwater, R.A. A Better Understanding of Vitamin E. Part 5: New Research Adds to Our Understanding. An Interview with Maret G. Traber, Ph.D. Whole Foods (September 2016) https://wholefoodsmagazine.com/columns/vitamin-connection/better-understanding-vitamin-e-2-2/
- For Heart Disease – Vitamin E. Ratcliff, J.D. Coronet (June 1948).
- Shute, W. E.; Shute, E. V.; et al., Alpha Tocopherol (Vitamin E) in Cardiovascular Disease. Toronto, Ontario, Canada: Ryerson Press, 1945.
- Vogelsang A, Shute EV; Shute (June 1946). "Effect of vitamin E in coronary heart disease". Nature 157 (3997): 772. Bibcode:1946Natur.157..772V. doi:10.1038/157772b0. PMID 21064771.
- Shute EV, Vogelsang AB, Skelton FB, Shute WE; Vogelsang (January 1948). "The influence of vitamin E on vascular disease". Surg Gynecol Obstet 86 (1): 1–8. PMID 18920873.
- Skelton F, Shute E, Skinner HG, Waud RA; Shute; Skinner; Waud (1946). "Antipurpuric Action of A-Tocopherol (Vitamin E)". Science 103 (2687): 762. doi:10.1126/science.103.2687.762-b. PMID 17836459.
- Passwater, R.A. Whole Foods pp 54-56 (October 1992).
- Passwater, R. Supernutrition For Healthy Hearts. Dial Press 1977.
- A. Passwater, “Heart Disease and Vitamin E Study,” Prevention 28 (1), 63–71 (1976). Also see Passwater, R. A., “Supernutrition For Healthy Hearts” Dial Press, NY (1977) and Passwater, R. A., “The New Supernutrition.” Pocket Books NY (1991).
- Press Conference. Prevention Magazine and Passwater, R. A. National Press Club. Washington, D.C. (December 24, 1975).
- Enstrom, J.E. and Pauling, L. Mortality among health-conscious elderly Californians. Proc. Nat. Acad. Sci. USA Vol. 79, pp. 6023-627, (October 1982).
- Rimm, E.B.,et al., “Vitamin E Consumption And The Risk Of Coronary Heart Disease In Men,” N. Engl. J. Med. 328 (20), 1450–1456 (1993).
- Stampfer, M.J.,et al., “Vitamin E Consumption And The Risk Of Coronary Disease In Women,” N. Engl. J. Med. 328 (20), 1444–1449 (1993).
- Gey, J. Fred, Puska, Pekka, Jordan, Paul and Moser, Ulrich K. Inverse correlation between plasma vitamin E and mortality from ischemic heart disease in cross-cultural epidemiology. Amer. J. Clin. Nutr. 53:326S-334S (Jan 1991).
- Riemersma RA, Wood DA, Macintyre CCA, Elton RA, Gey KF, Oliver MF. Risk of angina pectoris and plasma concentrations of vitamins A, C, and E and carotene. Lancet 1991;337:1-5.
- Sklodowska, M., Wasowicz, W., Gromadzinsks, J., et al. Selenium and vitamin E concentrations in plasma and erythrocytes of angina pectoris patients. Trace Elem. Med. 8:113-117 (1991)
- Bolton-Smith, C., Woodward, M. and Tunstall-Pedoe, H. The Scottish Heart Health Study. Dietary intake by food frequency questionnaire and odds ratios for coronary heart disease risk. European J. Clin. Nutr. 1992, 46(2):85-93.
- Bellizzi, M.C., Franklin, M.F., Duthie, G.G., and James, W.P. Vitamin E and coronary heart disease: The European paradox. Eur J Clin Nutr 1995 Mar;49(3):230.
- Knekt, P., Reunanen, A., Jävinen, R., et al. Antioxidant Vitamin Intake and Coronary Mortality in a Longitudinal Population Study. Am. J. Epidemiol. (1994) 139 (12): 1180-1189.
- Luoma PV, Nayha S, Sikkila K, Hassi J. High serum alphatocopherol, albumin, selenium and cholesterol, and low mortality from coronary heart disease in northern Finland. J Intern Med. 1995;237:49–54.
- Hodis, H.N., Mack, W.J., LaBree, L., et al., Serial coronary angiographic evidence that antioxidant vitamin intake reduces progression of coronary artery atherosclerosis. JAMA. 1995 Jun 21;273(23):1849-54.
- Singh, R.B., Ghosh, S., Niaz, M.A., et al. Dietary intake, plasma levels of antioxidant vitamins, and oxidative stress in relation to coronary artery disease in elderly subjects. Amer. J. Cardiol. 76:17;1233-1238 (15 December 1995).
- Torun, M., Avci, N. and Yardim, S. Serum levels of vitamin E in relation to cardiovascular diseases. J. Clin. Pharm. Thera. 20:6.335-340 (Dec 1995).
- Kushi, L.H., Folsom, A.R., Prineas, R.J., et al., Dietary antioxidant vitamins and death from coronary heart disease in postmenopausal women. N Engl J Med. 1996 May 2;334(18):1156-62.
- Losonczy, K.G., Harris, T.B., and Havlik, R.J. Vitamin E and vitamin C supplement use and risk of all-cause and coronary heart disease mortality in older persons: the Established Populations for Epidemiologic Studies of the Elderly. Am J Clin Nutr. 1996 Aug;64(2):190-6.
- Meyer, F., Bairati, I. and Dagenais, G.R. Lower ischemic heart disease incidence and mortality among vitamin supplement users. Can J Cardiol. 1996 Oct;12(10):930-4.
- Regnström, J., Nilsson, J., Moldeus, P. et al. Inverse relation between the concentration of low-density-lipoprotein vitamin E and severity of coronary artery disease. Am J Clin Nutr 63:3;377-385 (March 1996).
- K Kostner, K., Hornykewycz, S., Yang, P., et al. Is oxidative stress causally linked to unstable angina pectoris? A study in 100 CAD patients and matched controls. Cardiovascular Res. 36:3;330 – 336 (1997).
- Delport R, Ubbink JB, Human JA, Becker PJ, Myburgh DP, Vermaak WJ. Antioxidant vitamins and coronary artery disease risk in South African males. Clin Chim Acta. 1998 Nov;278(1):55-60.
- Adams AK, Wermuth EO, McBride PE. Antioxidant vitamins and the prevention of coronary heart disease. Am Fam Physician. 1999;60:895–904.
- Neuzil J, Weber C, Kontush A. The role of vitamin E in atherogenesis: linking the chemical, biological and clinical aspects of the disease. Atherosclerosis. 2001 Aug;157(2):257-83.
- Ashor, A.W., Siervo, M., Lara, J., Oggioni, C. and Mathers, J.C. Antioxidant Vitamin Supplementation Reduces Arterial Stiffness in Adults: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. J. Nutr. doi: 10.3945/jn.114.195826
- Food Nutrition Board, Institute of Medicine, Dietary Reference Intakes for Vitamin C, Vitamin E, Selenium, and Carotenoids (National Academy Press, Washington, D.C., 2000), www.ncbi.nlm.nih.gov/books/NBK225483, accessed June 13, 2016.
- Stephens NG, Parsons A, Schofield PM, Kelly F, Cheeseman K, Mitchinson MJ. Randomised controlled trial of vitamin E in patients with coronary disease: Cambridge Heart Antioxidant Study (CHAOS). Lancet. 1996;347(9004):781-786.
- Correia, M.L.G. & Haynes, W.G. Arterial compliance and endothelial function. Curr Diab Rep (2007) 7: 269. doi:10.1007/s11892-007-0043-1
- Ashor AW1, Siervo M1, Lara J1, Oggioni C1, Afshar S1, Mathers JC1. Br J Nutr. 2015 Apr 28;113(8):1182-94. doi: 10.1017/S0007114515000227.
- Effect of vitamin C and vitamin E supplementation on endothelial function: a systematic review and meta-analysis of randomised controlled trials.










